Can Mindful Eating Promote Behavior Change?
 Mindful eating can help reduce automatic and emotional eating.
Mindful eating can help reduce automatic and emotional eating.
Inattentive eating, sometimes referred to as automatic eating, is a learned behavior. Automatic eating occurs when we eat around mealtime, even in the absence of hunger. We are also at risk of automatic eating when we see food or have it readily available at arm’s length, e.g., the tempting candy bowl on a colleague’s desk or your coffee table.
Automatic eating also manifests as emotional eating, wherein one uses food as a way to cope with depression, stress, or sadness.3 When food is used as a coping mechanism to manage elevated states of negative arousal, it is likely to become habitual and automatic. This begs the question, what can be done to mitigate one’s automatic impulse to eat driven by habituation to mealtimes and easy access to food, particularly since obesity has been identified as the second leading cause of preventable death is associated with increased risks for type 2 diabetes and cardiovascular disease?
While successful weight loss can be achieved through traditional approaches such as diet and exercise, integrative approaches, or complementary approaches, have also been shown to support successful weight loss. Recent research suggests that integrating mindfulness-based interventions, such as mindful eating, may help promote behavior change in the context of eating behaviors and mitigate automatic and emotional eating.
Integrating Mindfulness and Mindful Eating into a Weight Loss Program
Mindfulness is defined as purposeful and non-judgmental attention to the present moment. Mindful eating, a form of mindfulness is an approach to food that is characterized by paying purposeful attention to our food, and it can disrupt automatic responses to food and inattention to emotional triggers that precipitate a habituated response to satisfying food cravings. Mindful eating has been reported to increase one’s sensitivity to hunger and satiety cues as well as one’s food environment, eating pace, and characteristics of the food being consumed. Mindful eating purposely directs our attention to the activity of eating and helps bring conscious awareness to the task of eating, which can mitigate habituated responses to food.
A recent review of studies that included mindfulness-based interventions centered on mindful eating found strong support for integrating mindful eating into weight loss programs. Although the research in this area is still new, compared to the body of research on traditional diet and exercise approaches to weight loss, consideration of integrating mindful eating practices into a weight loss program is warranted.
— By Dawn M. Sweet, Ph.D



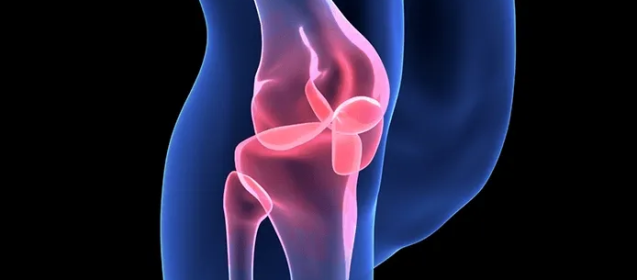
 Losing weight can reduce knee pain and improve the kinematic function of the knee. It is estimated that nearly one-third of adults with obesity have arthritis. Patients with obesity are at an increased risk of developing knee osteoarthritis because of the increased load placed on their knee joints. For example, a common estimate is that for every one pound of body weight, your knees experience the force of three pounds of pressure each time you take a step. This means that losing just 10 pounds will yield a 30-pound decrease in pressure on your knees for each step taken. For patients with obesity, an elevated joint load can lead to knee osteoarthritis, which is accompanied by gait alterations and can further affect pain.
Losing weight can reduce knee pain and improve the kinematic function of the knee. It is estimated that nearly one-third of adults with obesity have arthritis. Patients with obesity are at an increased risk of developing knee osteoarthritis because of the increased load placed on their knee joints. For example, a common estimate is that for every one pound of body weight, your knees experience the force of three pounds of pressure each time you take a step. This means that losing just 10 pounds will yield a 30-pound decrease in pressure on your knees for each step taken. For patients with obesity, an elevated joint load can lead to knee osteoarthritis, which is accompanied by gait alterations and can further affect pain.
 Although GI issues are commonly reported side effects of semaglutide (GLP-1) medications, there things you can do to help patients reduce and manage them.
Although GI issues are commonly reported side effects of semaglutide (GLP-1) medications, there things you can do to help patients reduce and manage them.